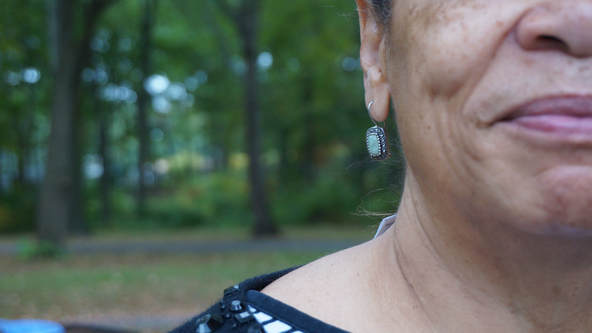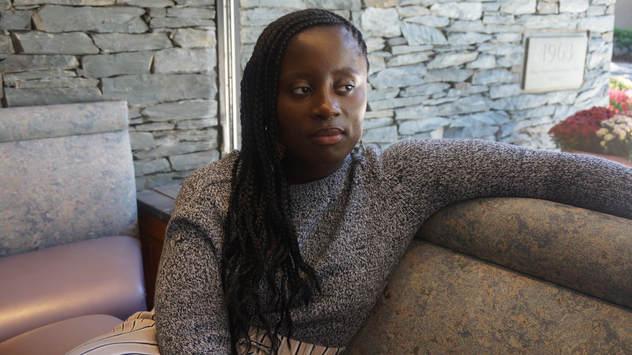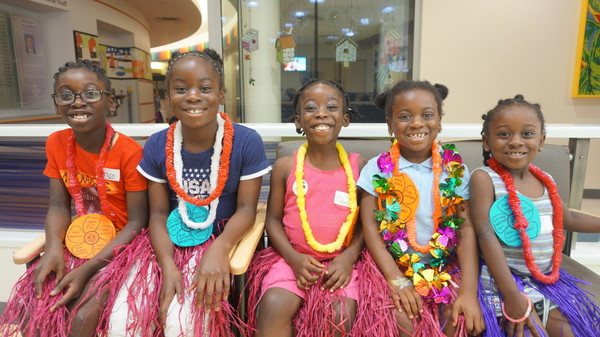|
“I think some people may think [sickle cell] is just a kind of anemia, but it's so much beyond that. This is a type of anemia that forces you to live with chronic pain that interferes with your day to day. Not only does it cause chronic pain, but it can interfere with your ability to breathe. Sickle cell is a hematologic condition, but it's a multi-organ condition. It causes complications with your lungs, kidneys, sometimes your nutritional status, and GI system. It's a complex disease. That's why I think it's really good for us as a community- patients, families, doctors, nurses, social workers- getting together and mobilizing to educate the public, get more funding, and more awareness. The hardest part is trying to build a multi-disciplinary clinic. If you're in different specialties, it's hard to get the green light to have space and time to do this outside our clinical homes. I think it's important for doctors from different specialties to talk to each other. It makes it easier for patients to see us all together, so they don't have to make separate visits. One of my dreams is to build a clinic where a lot of the providers will be in the same clinic. We learn from patients as doctors and we learn from other doctors. The best part of my career is getting to know patients and seeing them improve. It's hard when you have a patient who's not doing well and you feel like you've done everything you can. It's really hard, but the good side is when you see a patient improve.” (5b,5) (Pulmonologist, Connecticut Children’s Medical Center)
0 Comments
“I’ve always liked working with children. I also liked biology. As I got older, it seemed medicine would combine both of those things. In my residency program, I really liked the pulmonologists I worked with. They drew me in along with the patients they followed. It would not just be the doctor and the patient. The social worker would have a big role. The nurse specific to that patient population would have a big role. You have a whole team that is going on the journey with the child and trying to help them get better and enjoy life. [During a pediatric pulmonary conference], one of the speakers was a hematologist/ oncologist from California. He's done a lot of the initial research showing the link between asthma and sickle cell disease and how sickle cell disease affects the lung. He gave a really inspiring talk. At that point as a resident, I had taken care of a lot of kids who were admitted for pain crises or for acute chest. I would see the kids that had that pneumonia or bad asthma. When I saw a child with acute chest and they were struggling to breathe and they were also dealing with the pain, I wished there was something more to do then what we had to offer. Seeing this doctor talk made me think, "Maybe there is more we can do." I decided I wanted to do work specifically with pulmonology and sickle cell.” (5a/5) (Pulmonologist, Connecticut Children's Medical Center)
Wishing you a Happy New Year! Visit Visit us in January, 2018 to see our final Faces of Sickle Cell Strength feature.
“I'm a nurse at Connecticut Children's in the pulmonary department. I grew up in Jamaica and I knew a young lady that had sickle cell. It wasn't until I was 26 and pregnant with my first child that I found out I carried the trait, which was very shocking. Even though I'd been a nurse for four of five years, it wasn't on my radar to get tested for sickle cell. After finding out, I thought it was important to educate the folks around me. When my son was born, I was lucky that he only had the trait. For three months it was constantly on my mind. His father refused to get tested, so I had no idea if he was going to be born with the disease or with the trait. Unfortunately, my brother who also has the trait never got tested prior to my nephew being born. He was born with the full disease. Before he was three, he was intubated several times; he had acute chest several times; he had to have his spleen removed; he had to have a tracheal repair. It was really tough for my brother and his wife and also for us. I think it's really important for people to know their status. Part of my goal is to help educate the next generation, like my son, who is now 21, and his friends. I'm passionate about it. It's personal and I just hope that in the future, for my nephew who's four, there will be a cure in his lifetime.” (3/4) (Nurse, Connecticut Children’s Medical Center)
“I'm one of the nurse practitioners in pulmonary. I remember on one of my missions in Colombia there was a little girl. She was in clinic with her parents and something about anemia came up. I said, 'Has your daughter ever been tested for sickle cell?’. They looked at me like I was speaking a foreign language. I explained what it was. They were Afro-Colombian so I said, ‘You're more at risk. Let's just test her. You're already here in the hospital.’ I knew if she left she wouldn't have gotten the testing done. It came up that she tested positive for sickle cell. If I hadn't mentioned it, they would've gone unnoticed. I always think of her and what her life must be like now. I didn't know how prevalent and how underfunded it was until I started working in sickle cell. It's exciting to know there are new treatments coming out.” (2/4) (NP, Connecticut Children's Medical Center)
“I'm one of the respiratory therapists in the pulmonary lab. I was inpatient and I took care of many sickle cell patients in those 10 years. I came to outpatient five years ago. It's been really nice to expand my knowledge base about sickle cell. The outpatient world is very different. It's been a joy. I'm learning every single time we have clinic. We're doing some combined clinic with hematology/oncology. ‘
[I] was really impressed with the young man and his passion and maturity [at the Sickle Cell Family Advisory Board]. He wanted to do a fundraiser. He put a lot of thought into it and a lot of creative ideas. He was so brave and so courageous and so mature about it. It left an impact that he wanted to be so forward and want to make that change and educate. I thought it was beautiful at his age. I was impressed. The more you learn, the more you can share with people, the more you can talk about it with knowledge base. I think my biggest message would be to make sure to take care of your airways and to keep up with your respiratory therapy. Long term, it's extremely important to the health of your lungs.” (1/4) (Respiratory Therapist, Connecticut Children's Medical Center) “Because the disease was so new, they didn't know much. I got married. My husband found out he had the trait. I had the trait. My son was three years old. We had bought him some sneakers. He kept saying, ‘Mommy, my feet are hurting.’ We took him to the hospital. At one o'clock in the morning he kept saying,‘My legs are hurting.’ That's the day they diagnosed he had it. He was three years old. He was 42 when he passed away. He had one daughter. He was crazy about her. He died December 21st, 2014. It'll be three years from this December. They lived good, full lives. You couldn't slow them down.” (2/2)
"My mother had sickle cell. She came up from St. Louis, Missouri. They were treating her up in Connecticut for leukemia, but her doctor out of Germany said, 'It's not leukemia. It's sickle cell disease.' My mother was the first patient up here to be diagnosed with the correct name of it. My mom lived to be 58. She was one of the oldest living [with sickle cell] at that time. She's been deceased now for 27 years." (1/2)
“Sickle cell disease is awful, but a person who has sickle cell is not sickle cell disease. They're a person first and the disease just happens to come along. I've been doing this long enough that I get to watch my kids grow up. I've been the [volunteer sickle cell] doc at The Hole in the Wall Gang Camp for 15 years. Every time I go there's always something amazing that happens. Some stories that the kids tell or just their smiles even. I have pictures of all my kids when they go to prom. I’ve been to graduations. Those are all impactful. All the growing up stuff. I've been there when at least four of my girls have given birth. There's something about sickle cell disease that makes you understand and comprehend and empathize with everyone. They make amazing parents- watching them run record companies, watching them try to be division I athletes and succeeding. They can do anything just like everyone else. I think that's been the best part.
Watching people come around to support somebody through, that’s amazing, too. There's things that everyone could do whether they're in the medical field or not to help. As you're raising awareness, one of the simplest things to do is to give blood, especially if you're a minority person, or to offer to be a bone marrow donor, because transplants are the only cure at this point in time. There's a lot of hope for the future. For anyone with sickle cell disease, take care of yourself. Stay healthy, so when a cure comes you're all set.” (2/2) (MD, Hasbro Children’s) “I did my fellowship in San Francisco. I had the joy of working at Children's Oakland and got a lot more exposure. I always wanted to cure sickle cell. I really want to make this go away. It's a bad disease. We need to fix it. The hardest part being a physician working with sickle cell disease is people don't get it. Particularly insurance companies and some people in the community don't understand that you can be agonizing pain and have nobody recognize it or realize how bad it is. I think that's my frustration. I don't think it's true that nobody cares. I just think, sometimes, that unless you see it and you live it, you don't know what's actually going on.
I've only lost five patients to sickle cell disease. I've taken care of 200-300 kids and adults with sickle cell disease. It's the ones where they have died that have bothered me. One gentleman got to have his first child even though we thought he wouldn't be able to procreate children. His child was a year old. He got acute chest syndrome and died very quickly. Again, no fault of the system. Everyone did what they were supposed to do- including him, including his family. Sometimes no matter how hard you try, when you get acute chest bad enough, no matter how many transfusions you give, how quick you are, how compliant you are with the medicines- all the things he did right, and it still killed him. Those are the ones that hurt.” (1/2) (MD, Hasbro Children’s) “I'm a nurse. I've been a patient very briefly. I've been the family member and now I'm a healthcare professional. I'm seeing things full circle. I would say this to anyone. Take the time to learn more about sickle cell. I feel like people may think that they know, but they really don't know. Even if you do know, do you know enough that you're willing to do something about it? How many of us can say that we're on the registry or that we donate blood on a regular basis? If we really know about sickle cell, we will want to be active about changing the circumstance for sickle cell patients. I would stress to anyone hearing this to take the time to educate yourself. Recognize a lot of these patients have been on these medications since they were kids, so how they may be treated or affected differently is something we need to consider. I think all along this perspective, from a novice to an expert, there's still more we can learn.” (5/5)
“When you have someone that is sick, you can limit them. I feel like he fought against that, because he wanted a sense of normalcy like everyone else. At the same time, you need those people around you to say, ‘Think about this.’ Now that he's in college and he knows more about his disease, he's been proactive himself.
I think the thing I love most about my brother is that he's a fighter. No one can describe how they're feeling like they can. One time my brother said, "This is so painful. I feel like someone's stabbing me in the back, turning the knife, pulling it back out and stabbing me again over and over." I can't even comprehend what that feels like. He just shows us time and time again that he's able to overcome. I think that's really special and very unique to his story.” (4/5) “We always knew what the options were for curative treatments. When we started to have a discussion of [a bone marrow transplant] we had already done some blood work and we worked with Be the Match to find him a full match donor. We had tried over a year. I had held different drives through my college to help increase the chances of donors, but we still came up short. My mother spoke with my brother's hematologist. That's when it was brought to her attention that other hospitals nationally had been doing half transplants and they had been successful. The biggest challenge of it was finally making the decision. At the time he was a teenager in high school, so he had to realize that he was going to miss out on a good part of a crucial time in his life and try to figure things out for the future. All these things were up in the air. The final decision ended coming about as a family that it was worth it for us to try. When I found out I could be his potential donor, there was no debating for me. I was going to do what I could. It was in the later part of May in 2013. It was a big day. The whole family was there for the first two weeks.” (3/5)
“I think the hardest part was when I was in high school. I was volunteering at a local hospital and was interacting with a staff member. We happened to see someone who had sickle cell and the first thing she said was, 'They're all drug addicts.' When she said that I was completely taken aback. Just getting that mental image of all the things that my brother has been through and to see someone out of that picture judge someone in that state really hit me hard. It also brought to the light how there is a lack of understanding, even on the health professional side, that I had no awareness of up to that moment.” (2/5)
"He and I are four years apart. When I started to notice the effects of it, I was ten or eleven. He was young, maybe 7 or 8 years old. I remember him being in the hospital bed. He just looked so sick. His eyes were so yellow. At the time, he was a very adventurous kid. He didn't want to do anything. He was in a ball, crying, not able to be comforted in any way. I think that was the first time it hit me that he was really, really sick. I felt so sad that there was nothing I could do.
I think from a sibling role, I had a couple of options. I could either become inspired and involved or I could be like, 'It's not my problem. It's not my thing.' I chose the first option. My mom was very involved with trying to put events together for sickle cell patients. I jumped on board with her. Growing up, a lot of my projects had to do with things around sickle cell, whether it was projects in the community or just educating my peers or teachers about the disease." (1/5) "Challenges of medical social work are that people still have the stigma that if they're meeting with a social worker then they did something wrong. There's a stigma that 'I don't need to talk about my illness'. There's a link between your emotional coping and your pain. Then the resource piece of it is challenging. A lot of other diseases have more funding.
I'm sure most of my patients have had a moment of thinking 'What if I didn't have sickle cell?' Then you can have a good conversation about that and say, 'This is what you want. Why can't we make that happen?' My job is to help you get there or to put you in touch with the people that you should be. Getting to see some of these kids grow up and go to college, and some of them have gotten married and had babies and do all these things that you'd hoped when you met this little kid. I think that's one of my favorite parts about being in the hospital. Sickle cell disease should not define who a person is. It doesn't matter what your illness is. You should be able to be given every opportunity that every other person on this earth is given. We have to be more open-minded to how we're approaching people." (Social Work, Hasbro Children's) "The highlight of my career has been working overseas in Africa. We launched a newborn screening program in the country of Angola. Our team was recruited by the Minister of Health to come and launch this program. Our team worked really hard with the local people to get the lab up in place. Within twelve months we had diagnosed many patients. They coming into clinic. They were getting shots of penicillin. Their families were so engaged and so interested in learning about the disease and the steps they could take to prevent the complications. Overcoming some of the myths that we thought were there was definitely the most fulfilling part of my career." (PA, Hasbro Children's)
“Winter's a little tough, because he can't go outside in the snow like he wants to or play outside for recess. He's upset about that. His school is excellent with it. They try to help in anyway possible. He doesn't go anywhere without someone knowing that he has it. They all have to be aware of it, because he can have a crisis at any time. The sad part is a lot of people don't know about it. They just know it has something to do with the blood. That's my one main thing. That it needs to be out there. People need to be aware. He'll be 11. I'm still learning every single day. (3/3)
“I was out camping with my uncle and I had a really bad crisis at 2 o'clock in the morning. We were in Connecticut. We had to drive all the way back, move to my mom's house, and take care of me. It's hard. It gets annoying sometimes, because I can't do anything I really want to do. I like to play baseball, make food- all sorts of stuff. Desserts especially! My dream for the future is to become either a vlogger, a gamer, a business man, or a professional football player.” (2/3)
"I found out when he was two that he had sickle cell. I have Italian, Swedish, and Indian in me. His father is mixed as well. I carry the trait and his father carry the trait. I didn't know that until I found out [my son] had [sickle cell]. It was heartbreaking. He was buckled down to his knees crying in excruciating pain. He got pale. His eyes turned yellow. There's really nothing you can do, but pain meds.
When I found out I wasn't a match, that was even more heartbreaking. Knowing the fact you can't save your child's life is beyond devastating. The hardest part is knowing that he has to go through something the rest of his life that I can't really control, and knowing that there's no cure for it besides a bone marrow transplant. He's still young. As time goes on we're hoping there's some kind of cure besides this." (1/3) "My medical degree is from Aberdeen in the North of Scotland. I ended up choosing a fellowship in pediatric hematology/oncology. This was an area that needed people to go into. There's a suggestion that sickle cell disease is more palatable than oncology. The children with sickle cell have just as rough a time as oncology. To me, seeing them come in with yet another pain episode, yet another hit against them, makes me feel so sorry that they have an illness that does this.
I felt very uplifted when the mother of one of the patients I took care of when I was in Boston [Children's Medical Center] came to me after her daughter had been successfully transplanted from her little sister. To see the little girl and her mother and her little sister in that first clinic visit after she had been discharged was such a wonderful feeling that [she] no longer has the disease and we have cured her. It's that that I need in clinic everyday to feel that there's a best to it." (Hasbro Children's) "One of my dear friends lost her first born child to sickle cell when he was only 18 months. I had known about the disease and knew what could happen. I had heard her story and it touched my heart. I wanted to see if I could do anything to make a difference for anybody with sickle cell. I've been here over eleven and a half years. There's been quite a few times where I've seen [the kids] very sick. It's heartbreaking. It's amazing that I'm the one who'll stick them with needles, but they run and jump in my arms to give me a hug. It's very rewarding. I love seeing them. I don't know what else I would do if I wasn't a nurse." (Hasbro Children's Hospital)
"It has been a bumpy road at times. A few times she's had pain, been on a constant drip of pain medicine and still have the pain break through- unbearable to me was to read that the sickle cell pain is comparable to the labor pain. I know what the pain of childbirth is, and to think that a child that young, that little has to go through that amount of pain has made her pain real to me. Through it all, I've always taken a cue: first from God, I take courage from faith in Him: we have what it takes to go through and face whatever dares come our way in this imperfect world. Secondly from family, the support of family and friends in the throes of the crisis, lessens the weight of the load, and then thirdly, I look at her, how she deals with the series of procedures that are warranted because of the condition. Sometimes her only concern after so many sticks with a needle is that she gets her favorite color Band-Aid on the place where they poked her so many times. Her sisters have been wonderful when she’s not well. It affects all of us and we just rally together. It's made us a better family. We can only face it together, and we have wonderful external support that's been family and friends. We've learned to enjoy the moments when it's good, and when it's not so great, we still make the most out of it. Having good support has been a vital part of this journey. The folks at Connecticut Children's have been phenomenal. They make it bearable during the difficult times, so I'd like to thank them for all they do." (5/5)
"It doesn't feel good to have one of your sisters at the hospital, because all of us aren't together at home. It can be rough. I feel sad and sometimes I cry. Sometimes when we're playing outside with our friends, she's inside taking her medicine. When Hadassah's there with us it really adds to the fun, so we're always sad when she can't come and play with us.
Good things I like about Hadassah are how she's creative and unique and how she likes to help with different cooking things in the kitchen. My favorite thing to do is puzzles with my sister. My favorite thing about Hadassah is [when] we all jump together. Since I want to be a doctor or nurse when I grow up, I like to help her with her medicine and help her get around. Sometimes we make her breakfast and bring her water to drink when she's on the couch. I remember when she had her liver biopsy. I went with her and was kind of like her nurse while she was in recovery. Whenever Hadassah's at the hospital [and] she comes home- even though some not so good things happen there because she went there because she was sick- she also tells us about the good things that happen and how she gets prizes. When she comes home and tells us those things, we know the doctors are treating her well. There is also a songwriter and her name is Jamie-Grace. Hadassah really loves listening to her songs. Whenever she's at the hospital she listens to her songs. It gives her hope and courage to keep on going until she's able to come home. Hadassah's favorite song by Jamie Grace is "With You". I think that it almost feels like she's there with her." (4/5) |